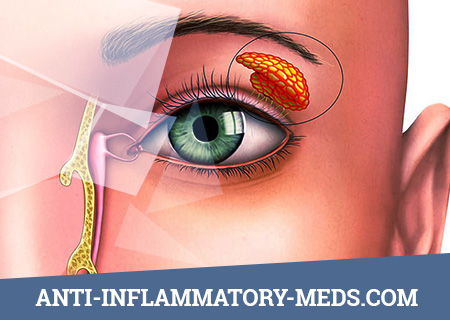
The Clinical Picture
Xerophthalmia, i.e., dry eye itself, associated with insufficient tear formation, usually serves as the first sign of illness. Patients complain of dry eyes, a foreign body (“sand”), burning, itching, pain, discomfort when reading, difficulty opening eyes in the morning, photophobia. On examination, the eyes look irritated, dry, with the expansion of the conjunctival and pericorneal vessels. A characteristic small amount of a tiny or thick viscous discharge is white or yellow. Patients have reduced tearing down to the complete absence of tears, which is especially noticeable with severe negative emotions (inability to cry) and exposure to irritating substances (in particular, the absence of tearing during onion cleaning). As a rule, patients feel better in areas with a humid and cool climate.
An objective diagnosis of dry keratoconjunctivitis is possible when stained areas of the conjunctiva and cornea are stained with 1% Bengal pink solution (the results of this technique, however, are not always interpreted unambiguously) and especially with the help of a slit lamp, which makes it possible to reliably establish point and filamentous keratitis. To recognize reduced lacrimation, the most popular Schirmer test is as follows. A strip of filter paper 5 mm wide is laid with its upper end behind the lower eyelid at the border of its middle and inner third. Normally, the paper gets wet for 5 minutes at least 15 mm. With lower results, tear secretion can be stimulated by inhalation of a 10% solution of ammonium chloride, the bottle with which is placed 15 cm below the nose (“forced Schirmer test”). A positive Schirmer test (i.e., the very fact of insufficient tearing) is not synonymous with dry keratoconjunctivitis, especially if this study is carried out at high temperature in a dry room.
A clinically noticeable increase in the lacrimal glands in Sjogren’s syndrome occurs in no more than 5% of patients. Dry eyes in this disease cannot be associated only with the destruction of the parenchyma of the lacrimal glands by inflammatory infiltrate, since the surgical removal of these glands (for other reasons) does not lead to such pronounced dryness. Apparently, the defeat in the development of xerophthalmia is also affected by Sjogren’s syndrome of all the mucous glands of the conjunctival sac. Possibly, a change in the biochemical composition of tears can play a role: a decrease in viscosity and an increase in water content make it impossible to create an even layer of tears over the surface of the cornea.
Untreated dry keratoconjunctivitis can be complicated by a secondary infection, which is associated primarily with the weakening or absence of the bactericidal action of lysozyme, contained in the normal secretion of the lacrimal glands. Multiple complications are possible as a result of an infection (bacterial or viral) – eyelid fusion with an eyeball, loss of a blinking reflex, ulcerative keratitis, perforation of the cornea with the threat of uveitis, secondary glaucoma and loss of vision, which is very rare.
Xerostomia, if it exists in isolation, should not be considered as a mandatory manifestation of Sjogren’s syndrome. Dry mouth is observed in older people, alcohol addicts, smokers and people who breathe through their mouths or take antidepressants. Temporary severe dry mouth also occurs with nervous excitement. In addition, patients with Sjogren’s syndrome can experience only a very modest sensation of dry mouth and therefore do not actively complain about them. Moreover, even with indisputable histological signs of the disease, the amount of saliva sometimes remains sufficient so that the patient does not experience discomfort.
Severe xerostomia with Sjogren’s syndrome can be very painful. The greatest difficulties arise when chewing and swallowing solid food, in connection with which patients are forced to constantly drink it with water. Attempts to combat dryness by sucking lemon or sour candies are successful only in the early stages. In severe cases, food particles “stick” to the gums, cheeks and palate, and patients are forced to remove them with their hands. Dry pharyngeal mucosa can cause dysphagia; in some cases, a true violation of the mobility of the esophagus was noted.
Painful fissures of the lips and corners of the mouth are very common. The mucous membrane of the mouth is often irritated, its surface tissue is easily exfoliated, taking hot or spicy food causes pain. When milk is consumed, its curled threads lingering on the mucous membrane of the cheeks are sometimes misinterpreted as fungal lesions (which in some cases can indeed complicate xerostomia in Sjogren’s syndrome). Often painful atrophic glossitis with cracked tongue. Ulcerative stomatitis is also possible. Normal accumulation of saliva at the base of the frenum of the tongue in clinically expressed cases is not observed. It is also not possible to enhance salivation after massage of the parotid and submandibular glands. In most patients, the enlargement of the parotid glands is one-sided and temporary, although it is possible to maintain normal sizes as well as a bilateral increase. The submandibular glands are enlarged less frequently. Enlarged salivary glands are often slightly painful on palpation and, as a rule, are dense, with a smooth or uneven surface. At the same time, the stony density or nodularity characteristic of tumors is unusual for them. Acute pain in the glands, combined with fever, local hyperemia and hyperthermia, most often indicates the attachment of a secondary infection, which is usually the result of the often observed expansion and tortuosity of the intragland salivary ducts. To judge the pathology of these ducts, as well as the degree of atrophy of the parenchyma of the gland, contrast sialography can be successfully used. The severity of destruction of the glandular parenchyma is also determined by scintigraphy using labeled technetium (99mTe). In this case, the level of absorption of the radionuclide by the tissues of the salivary glands and, as a control, the thyroid gland is compared. It is peculiar that the amount of saliva allocated per unit of time, which, it would seem, should characterize xerostomia with particular accuracy, is in fact not a sufficiently reliable indicator, since it is subject to sharp individual fluctuations. For a general judgment on the reduction of salivation, it is sometimes important to verify the small stimulating effect of acidic foods, such as lemon.
With insufficient saliva, gingivitis, bad breath, tooth decay are common. The teeth crumble easily; previously placed fillings fall out of them. It should be borne in mind that xerostomia caused by drugs almost never causes dental pathology.
Changes in the mucous membranes of the external genitalia. The apocrine glands of the female external genitalia are often affected by Sjogren’s syndrome, which is accompanied by dryness and atrophy of the vaginal mucosa. Patients complain of dryness, burning sensation and dyspareunia. A histological examination often reveals nonspecific vaginitis. The interpretation of these changes is hampered by the fact that they are more often recorded in women during menopause and therefore may be a consequence of estrogen deficiency, and not dry syndrome per se.
Systemic manifestations of Sjogren’s syndrome often present serious difficulties in their pathogenetic interpretation. They can:
- to be symptoms of specific connective tissue diseases, with which Sjogren’s syndrome is very often combined;
- reflect the actual pathogenetic features of the syndrome in question;
- be a nonspecific consequence of the insufficient function of exocrine glands with dry mucous membranes, etc.
Obviously, the first category of symptoms does not apply to Sjogren’s syndrome as such and is not considered in this section.
Skin changes. A frequent sign of Sjogren’s syndrome is dry skin, although patients relatively rarely complain of it actively. In most patients, an increase in ambient temperature, physical activity or injections of pilocarpine cause noticeable sweating. However, in some cases this does not happen, and skin biopsies reveal inflammatory changes in the area of sweat glands with the destruction of their structure. Dermal. changes reflecting vasculitis (ulcers, hemorrhages) are discussed below.
Hives are often observed, which is a reflection of drug allergy inherent in Sjogren’s syndrome. C. Whaley et al. even found that allergic reactions to penicillin in RA are almost exclusively found in patients with concomitant Sjogren’s syndrome.
Damage to joints and muscles. From 50 to 70% of all patients with Sjogren’s syndrome have a concomitant inflammatory connective tissue disease (usually RA), which determines the nature of the articular pathology. However, among patients with primary Sjogren’s syndrome, 10-15% also have arthralgia or arthritis that do not fit into the clear framework of any specific concomitant nosology. Arthritis in this case is usually mild and transient. Despite the possible recurrence, erosion does not occur. The reverse development of inflammatory changes occurs without treatment. The most commonly affected are the knee and elbow joints. The pathogenesis of this arthritis variant is unknown. There is an opinion about its immunocomplex nature. An indirect argument in favor of this point of view is the frequent combination of Sjogren’s syndrome and RA, each of which is characterized by a high level of circulating immune complexes and the practical absence of dry syndrome in patients with psoriatic arthritis and other seronegative spondylitis, for which the formation of immune complexes is completely uncharacteristic.
It should be borne in mind that although in most patients with a combination of RA and Sjogren’s syndrome, the signs of the rheumatoid process long precede the dry syndrome, inverse relationships are possible. Therefore, with the first appearance of articular symptoms in a patient with prolonged isolated Sjogren’s syndrome, the onset of true RA cannot be ruled out.
Severe muscle damage in the primary Sjogren’s syndrome is almost not found, there are only a few relevant descriptions. Patients in some cases complain of mild myalgia and moderate muscle weakness, the latter may also be associated with electrolyte disturbances and tubular acidosis. Muscle biopsies in patients with primary Sjogren’s syndrome often reveal clinically asymptomatic focal myositis with perivascular lymphoid infiltration, as well as deposition of immunoglobulins and complement in muscle tissue and degenerative changes in myofibrils by electron microscopy.
Respiratory system. Almost 50% of patients with Sjogren’s syndrome note dry nasal mucous membranes. In some cases, it is significant and is accompanied by the formation of painful hard crusts and nosebleeds. Gustatory and olfactory sensations may weaken or change. On examination, atrophy of the nasal mucosa is found in many patients. Dry vocal cords are sometimes noted, on which there may be overlays of viscous mucus. These changes lead to hoarseness. A sharp decrease in hearing and serous otitis media are possible due to the closure of the nasopharyngeal opening of the auditory tube with dry crusts; removal of crusts can lead to rapid improvement.
The so-called dry bronchitis is frequent, in which a thick mucous discharge causes a constant dry cough with difficulty in expectoration and the attachment of a secondary infection. In the development of the latter, insufficient local IgA production is also attached to a certain value. Relatively specific for Sjogren’s syndrome are considered infiltrates of the walls of the bronchioles and alveolar septa with T and B lymphocytes, which can be clinically manifested both by symptoms of airway obstruction with coughing and shortness of breath, and episodes of usually mild interstitial pneumonia. Often described light short-term pleurisy, self-resolving within 1-2 weeks. Chronic interstitial inflammatory process (fibrosing alveolitis) is relatively rare.
The cardiovascular system in Sjogren’s syndrome does not undergo any specific pathological changes, primarily associated with this disease.
Pathology of the kidneys. In a number of patients with Sjogren’s syndrome, latent or overt signs of impaired renal tubule function, manifested by tubular acidosis, aminoaciduria, and renal glucosuria, were detected. The mechanisms of development of these disorders are not fully understood. There is, in particular, the assumption that they are associated with chronic pyelonephritis or with increased blood viscosity as a result of hyperglobulinemia, often characteristic of Sjogren’s syndrome. It is more likely that this pathology is directly related to immune reactions, since in the corresponding patients, the medullary layer of the kidneys is infiltrated by lymphocytes and plasma cells. This point of view is supported by the fact that tubular acidosis in Sjogren’s syndrome decreases after treatment with cytostatic immunosuppressants. In addition, it draws attention that with autoimmune rejection crisis of a transplanted kidney, tubular acidosis also develops in combination with peritubular lymphoid infiltration. Since involvement of the tubules in the process can manifest itself in a decrease in the response to antidiuretic hormone, then while taking an increased amount of fluid (due to xerostomia), it sometimes leads to the development of a symptom complex of diabetes insipidus.
In rare cases, patients with Sjogren’s syndrome experience acute glomerulonephritis, combined with hypocomplementemia and deposition of immunoglobulin glomeruli and complement in the main membrane. It is important to note that this does not mean concomitant SLE, in which the development of Sjogren’s syndrome is quite real, since none of these patients had antibodies to native DNA that are highly specific for patients with lupus nephritis.
Digestive and abdominal organs. Dryness of the mucous membrane of the esophagus, which occurs with severe Sjogren’s syndrome, can cause mild dysphagia in some patients with solid food. Often chronic atrophic gastritis with markedly reduced acidity, sometimes combined with the presence of antibodies to parietal cells. In some patients, acute pancreatitis is described. Serious intestinal pathology and intestinal absorption disorders are not observed.
A slight increase in the liver and spleen in combination with moderate laboratory signs of impaired liver function is not so rare. Antibodies to mitochondria, smooth muscles and membranes of liver cells are relatively often found, which is considered a definite indication of the participation of the liver in the immune pathological process. The possibility of developing a specific hepatic pathology (chronic active hepatitis or primary biliary cirrhosis) as a manifestation of exactly Sjogren’s syndrome (as pointed out by some authors) does not seem to be sufficiently convincing. In such cases, the reverse causal relationship cannot be ruled out, since the secondary Sjogren’s syndrome often occurs in the aforementioned autoimmune diseases (similar to joint damage with RA, joint damage cannot be considered a manifestation of Sjogren’s syndrome). Among possible endocrine pathologies, histological signs of chronic thyroiditis of the Hashimoto type should be indicated in approximately 5% of patients with Sjogren’s syndrome. The autoimmune nature of both syndromes makes this combination understandable. At the same time, clinical signs of hypothyroidism are very rare.
In a number of patients with severe Sjogren’s syndrome, vasculitis of medium and small vessels is observed, which is manifested clinically by skin ulcers and peripheral neuropathy. It is characterized by a particularly frequent combination with the presence of Roantibodies. In a number of patients, vasculitis is combined with hyperglobulinemia and is possibly a reflection of immunocomplex pathology (at least in some cases). Its main symptom is “hyperglobulinemic purpura”, manifested by foci of hemorrhage on the legs. Elements of hemorrhage in typical cases are accompanied by itching and protrude above the surface of the skin, the temperature of which is usually somewhat elevated. In rare cases, the rash appears to be confluent. Hyperglobulinemic purpura is very characteristic of dry syndrome. It is believed that among patients with a combination of hyperglobulinemia and leg hemorrhage, 20-30% have or develop typical manifestations of Sjogren’s syndrome. Even with primary dry syndrome, Raynaud’s syndrome is more common than in the general population. However, his relationship with vasculitis itself seems dubious.
Changes in the central nervous system and cranial nerves by most authors are explained by vasculitis of the corresponding localization. A wide range of cerebral symptoms is described, including nystagmus, recurrent hemiparesis and, in especially severe cases, serous meningoencephalitis. Among cranial nerves, trigeminal with the development of a characteristic pain syndrome is relatively more often affected. In single patients with Sjogren’s syndrome, severe necrotic arteritis was observed with clinical manifestations corresponding to classical polyarteritis nodosa. However, it cannot be ruled out that polyarteritis in such cases was not a manifestation of Sjogren’s syndrome, but a “concomitant” disease (like RA and others).
Oncological complications. Compared with the general population, patients with Sjogren’s syndrome (especially primary) often have malignant tumors, primarily salivary gland lymphosarcomas. It is possible that the basis for the development of this pathology is the initial increased proliferative activity of B cells, during which a high probability of occurrence of mutations is created. In combination with the attenuation of cellular immune responses discussed below, this fact can significantly facilitate the development of tumors. Between the usual lymphoid infiltration of the salivary glands and lymphosarcoma, there is, as it were, an intermediate stage called pseudolymphoma. In the corresponding patients, the salivary glands, lymph nodes and spleen increase, Hyperglobulinemic purpura, benign lymphoid infiltration of the renal tissue develop. Although steroid therapy can reverse these changes, they are considered a precancerous condition. Such patients should be monitored closely with early biopsies, especially in cases of rapid increase in the size of the lymph nodes and spleen. In addition to histological changes in biopsy samples, a decrease in previously elevated levels of serum globulins and the appearance of monoclonal immunoglobulins can also indicate a malignant transformation of the process. Attention is drawn to an increased risk of developing lymphosarcomas after radiotherapy of enlarged parotid glands. In addition, with Sjogren’s syndrome, more frequent development of skin cancer is noted.
Immunological characteristics of Sjogren’s syndrome. A characteristic feature of dry syndrome is hyperglobulinemia. It is especially pronounced in patients with primary Sjogren’s syndrome, causing in some cases the clinical manifestations of hyperglobulinemic purpura and a symptom complex of increased viscosity. In most cases, the level of several or all classes of immunoglobulins is elevated. These patterns, combined with the ability of lymphocytes from salivary gland biopsies to secrete immunoglobulins in cell culture, led to the idea of nonspecific B-cell activation in Sjogren’s syndrome. Such activation largely explains the high frequency of formation of the autoantibodies and immune complexes discussed below, as well as the tendency to lymphoproliferative reactions.